- Home
- Treatments
- Dental Treatments
Dental Treatments
-
Restorations
It is the way to restore the original shape and function of a decayed tooth. After removing the affected area of a decayed tooth, the cavity is filled with a restorative material. It restores the tooth original shape and function.
What is tooth decay?
Carbohydrates serve as food for bacteria in plaque which produce acids that destroy the tooth surface. Over time, tooth enamel begins to deteriorate, while th tooth surface while may remain intact. When this layer disappears, the surface collapses exposing the cavity. Dental Cavities develop most often in the fissures of the occlusal surfaces of posterior teeth, between teeth and along the gumline. But no matter where they occur, the best way to detect and treat before they become a more serious problem is through a regular visit to the Dentist and Dental Hygienist is important to find early signs of decay and disease, it can help you mantain optimal oral health and prevent many dental problems.
How to prevent tooth decay?
By brushing after meals and flossing daily;
Regular dental visits;
Balanced diet (limiting the consumption of sugars).Aesthetic Restorations
Fractured teeth are restored using composite with the color of the remaining teeth. It is used a clear tape is used to separate the teeth and by adding the composit resin to the fractured tooth, it can be sculpted and it's function and aesthetic restored. After the tooth is sculpted the material is hardened by applying a strong blue light.
A diastema is a space or gap between teeth. It appears more often between the two upper front teeth. However, gaps can occur between any two teeth. There are several treatment options for closing spaces depending on the patient, such as orthodontic treatment, crowns or composite resin restorations. A simple technique to resolve this problem is through composite resin restorations, where you can change the shape, contour and position of teeth. This type of restoration has the advantage of not requiring tooth preparation, making it the most conservative option.
Before

After

-
Endodontics
Consists of removal of dental pulp (nerve and blood supply), which is located in the center of the tooth, followed by instrumentation and filling with a biocompatible material.
When should it be done?
Due to caries or trauma affecting the pulp. When the pulp is infected an infectious process may occur causing pain and an abscess. Signs to look for include: pain, prolonged sensitivity to heat or cold, discoloration of the tooth, tenderness to touch and chewing, swelling. Sometimes, however, there are no symptoms.How is it done?
It is usually performed in multiple visits. During root canal treatment, the inflamed or infected pulp is removed and the root canal is carefully cleaned and desinfected so that it can be filled with a biocompatible material. Between the appointments a temporary restoration is placed to cover the opening of the crown. At the following appointment the root canals are filled and sealed definately with a rubber like material called gutta-percha.
Afterwards, the tooth is restored. In some cases where the remaining tooth structure is fragile, it may be necessary a fiber post to support the restoration or in more severe cases a crown may also be needed. After restoration, the tooth continues to make a crown.With proper care, most teeth that have root canal treatment can last as long as other natural teeth.
Before

After

-
Periodontal treatment
Refers to the treatment of gum disease.
What is gum disease?
Corresponds to an inflammation of the gums that can progress and affect the bone that surrounds and supports teeth. It is caused by bacteria in plaque which is a sticky, transparent film that constantly forms on teeth. If plaque is not removed by brushing and flossing, it builds up and can infect not only the gums but also the bone that supports the tooth, leading to mobility and tooth loss.
There are two main types of gum disease: gingivitis and periodontitis.
What is gingivitis?
Corresponds to inflammation of the gums. Clinically, the gingiva becomes very red and swollen. Brushing usually cause bleeding. This stage of gum disease is reversible because the alveolar bone has not been affected yet.
What is periodontal disease (periodontitis)?
Gum disease when left untreated can progress to periodontal disease. This affects the supporting tissues of the tooth leading to mobility and even tooth loss.
How is gum disease treated?
The early stages of gum disease may be reversible with appropriate brushing and flossing. Good oral hygiene will help prevent forming plaque.
Periodontal scaling done in a professional office is the only way to remove plaque that has formed and calcified, forming tartar. The dentist / hygienist will remove tartar on the teeth and under the gum line. If your problem is more serious may need a root scaling. A root scalling smooths irregularities on the roots of your teeth making it difficult to grip the plaque.Gingival recession
Periodontal disease can cause gum recession, exposing the root of the tooth. The root is not covered with enamel so cold stimuli, warm and sometimes sweets can cause pain. A product can be applied to help this sensitivity.
-
Extractions
When does a tooth have to be extracted?
When decay has reached deep into the tooth and the infection has destroyed much of the tooth and surrounding bone or there is no space in the dental arch. Impacted or partially erupted teeth should be extracted and placed in the arc because food debris and bacteria can enter the area surrounding the partially erupted tooth can cause infection or impacted teeth can develop cysts intraosseous. Impacted teeth despite not having space to erupt they will continue trying to break through the gum may cause injury to adjacent teeth.
How is a tooth extracted?
The area around the tooth is anesthetized, with a tool (sindesmotomo) the gum is separated from the tooth, then another instrument (the lever) allows to release he tooth from the bone surrounding it and ultimately the tooth is removed with forceps. You may need suturing.
What are the precautions after a tooth extraction?
The dentist will ask the patient to bite on gauze for 30 minutes to limit the bleeding while the clot is formed. On the day of extraction the pacient should not smoke or rinse liquids, hot foods and avoid strenuous physical exercise. You may experience pain or discomfort after the extraction therefore your dentist will prescribe medication to combat this. You can also put ice in 15-minute intervals to minimize pain and inflammation. In the following days should gargle with an antiseptic solution (chlorhexidine) three times a day after brushing. Typically, the discomfort after dental extraction has improved 3-5 days. In case of persistent pain, swelling, bleeding or fever after 24 hours, the patient should seek a dentist.
What complications may occur?
Infection can occur but this usually does not occur when the immune system is healthy.
A common complication is to drought alveolitis that occurs when a clot is not formed or when it breaks prematurely, exposing the bone in the oral cavity. It is potentially painful.Sometime after a tooth extraction, bone and gums can change its shape leading to a change of position of the remaining teeth.
Wisdom teeth should be extracted?
Wisdom teeth are the last teeth on each side of the jaws and usually erupt at around 16-20 years. Since they are the last teeth to erupt many times there is no room for them in the arcade, and may be impacted.
-
Removable Prostheses
They are designated like this because they can be removed and reinserted in the mouth. They replace missing teeth, providing support for cheeks and lips. Without this support a person appears older reducing the ability to speak or eat. May be total or partial, according to the presence / absence of teeth. Are performed starting from molds made from the person's mouth.
It is important to note that the removable prostheses over time may become maladapted because the bone and gums are going backwards. Another solution is rehabilitation with fixed prosthesis or implants.
How are Dentures made?
Conventional Dentures are made after the extraction of teeth and tissue healing, which takes several months. During this period the person is without teeth. Immediate Dentures are held starting with the molds of the mouth in a prior consultation before dental extractions. The prosthesis is inserted immediately after teeth are extracted. Immediate dentures have the advantage of people never being without teeth, however, may be maladapted shortly after the healing process because there is a remodeling of bone that support the teeth. Dentures can be total when there is total absence of all teeth and are made of acrylic or partial when there are some teeth present and could be acrylic or skeletal.
How much time is needed to adapt to dentures?
It may take some time (weeks or months) until the person feels comfortable with the new prostheses. Initially it is normal to have a sense of 'mouthful', excessive saliva or mucosal irritation.
Caring for dentures?
Brushing your dentures daily to remove food remains and plaque. Brushing with a different brush (soft), the teeth or gums (stimulates blood circulation). Place a cleaning solution or water when not using it. Be careful when handling dentures because they may fracture if they fall.
After some time the prosthesis may become maladapted, and shall then be rebased or new dentures made.
Before

After

-
Fixed Phrostodontics
Crowns and fixed bridges are restorations that are cemented on teeth or implants and can not be removed except by a dentist.
What are the situations indicated?
When the tooth to restore is very broken, fractured, serve as a pillar of a bridge, has change of color or form or to rehabilitate a dental implant.
What are fixed bridges?
Are used to replace one more missing teeth. Bridges are cemented on natural teeth or implants, and these portions of the bridge are called abutments. The tooth to be restored corresponds to the pontic.
How to make a crown/bridge?
It may be necessary to perform endodontic treatment of teeth that will be prepared depending on the situation, not every tooth needing a crown need root canal treatment.
First the tooth / teeth are reduced and prepared for the crown / bridge fit perfectly. In this consultation is adapted a temporary crown/bridge that has an aesthetic and functional role to protect the tooth and gum.
Then a mold is made of the tooth and chosen the color for rehabilitation. This is send to the laboratory where they will manufacture the crown / bridge. When ready it will be cemented in the tooth / teeth.
What is the longevity of a crown/bridge?
It may last several years and this durability is closely related to the hygienic care of the patient. With time, the gums may recede and move away from the edge of the crown. It makes visible the termination of the crown which usually has a dark color due to the metal. The crown may be removed and made a new one more adapted to the gums consequently with more favorable aesthetics.
Before
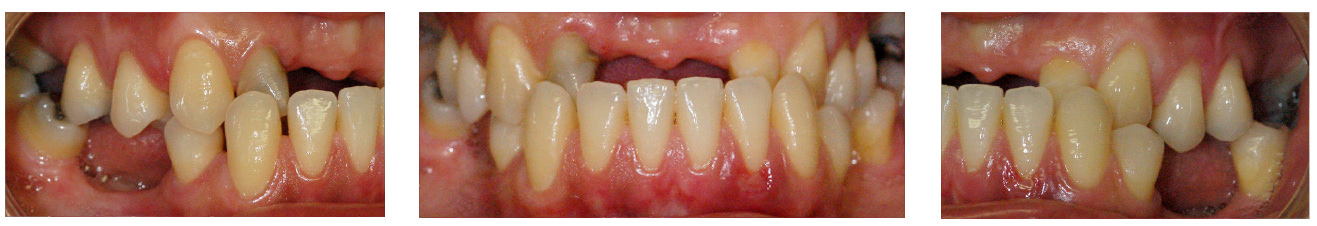
After

-
Whitening
What affects the color of teeth?
The color of teeth may be affected by many factors and of course some people have yellower teeth than others. The teeth may have surface stains (extrinsic) or internal (intrinsic). Surface stains are caused by tobacco, coffee, tea or red wine, highly pigmented foods or tartar. Internal stains can be caused by tetracycline (antibiotic), aging or dental trauma.
How is the whitenning process?
There are two main types of bleaching. When the bleaching is done in a tooth that was treated endodontically (the nerve is not alive) - Non-vital bleaching. When the tooth is alive - vital bleaching.
Preparation
f the patient has cavities they should be treated before bleaching. Should also do a scaling. Note that if the roots of the teeth are exposed they will not whiten as they are not covered by enamel. If the patient has restorations, they will also not bleach so it may be necessary to replace them after bleaching.
Bleaching non vital
The vital bleaching may not enhance the appearance of a tooth that has undergone root canal treatment. In this case the dentist uses a different procedure that whitens the tooth from within. The bleaching agent is placed inside the tooth and a provisional restoration is made. This is left for a few days repeating the procedure until the desired color is achieved.
Bleaching vital
The most common vital bleaching is done at home. Place a whitening gel (usually containing hydrogen peroxide) in a tray done from the model of the patient. This tray must be thoroughly adapted to the teeth for the whitening agent to be in contact with the teeth but not with the gum (the whitening agent is irritating to the gums). The tray is placed in the teeth for a few hours every day.
The vital bleaching can also be done in the office. The number of consultations will depend on each case and the desired color. A gel is applied to protect the gums followed by the whitening agent. Some whitening agents need to be activated with ultraviolet light.
Before
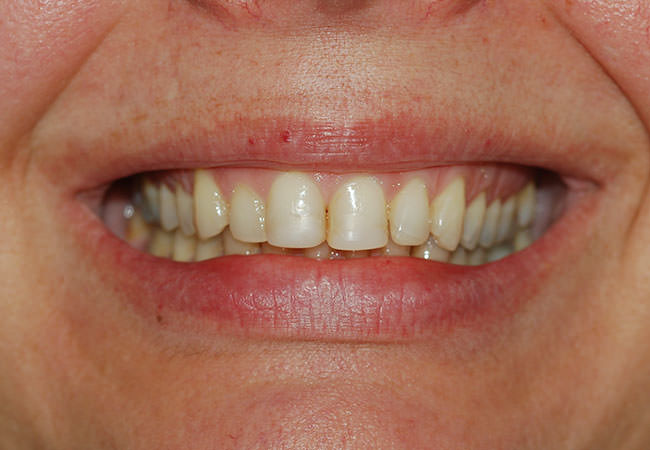
After

-
Oral Hygiene
In a oral hygine consultation the hygienist performs scaling followed by polishing and sometimes application of fluoride. It is taught the oral hygiene techniques appropriate to each patient.
Maintaining good oral hygiene is very important for the health of the mouth. Good oral hygiene corresponds to clean teeth without food debris and pink gums that are healthy and do not bleed when brushing or using dental floss.
How to maintain a healthy mouth?
 Brush your teeth after meals with a fluoride toothpaste
Brush your teeth after meals with a fluoride toothpaste Use dental floss daily, or swab stick interdental
Use dental floss daily, or swab stick interdental Make healthy eating
Make healthy eating
Tooth brushing technique: You should choose a soft brush with preferably a small head it comes more easily to all areas of the mouth.
You should choose a soft brush with preferably a small head it comes more easily to all areas of the mouth. Tilt the brush at a 45 degree angle against the gums to make horizontal movements, like see-saw or circular, with the brush from the gum line.
Tilt the brush at a 45 degree angle against the gums to make horizontal movements, like see-saw or circular, with the brush from the gum line. Gently brush the outer, inner and chewing surfaces of teeth making short moves coming and going.
Gently brush the outer, inner and chewing surfaces of teeth making short moves coming and going. Brush your tongue gently to remove bacteria and freshen your breath.
Brush your tongue gently to remove bacteria and freshen your breath.Technique using dental floss:
 Use about 45 inches of floss, leaving 3 or 4 inches of wire to work.
Use about 45 inches of floss, leaving 3 or 4 inches of wire to work. Hold the stretched thread between your thumbs and index fingers and slide it gently up and down between your teeth.
Hold the stretched thread between your thumbs and index fingers and slide it gently up and down between your teeth. Gently, make a wire around the base of the tooth , making sure it goes below the gumline. Never make a sudden movement or force the floss because it can cut or hurt the gum tissue which is very delicate.
Gently, make a wire around the base of the tooth , making sure it goes below the gumline. Never make a sudden movement or force the floss because it can cut or hurt the gum tissue which is very delicate. Use clean sections of floss as it passes from one tooth to another.
Use clean sections of floss as it passes from one tooth to another. To remove the floss, use the same moves forward and backward, as the floss goes away from the tooth.
To remove the floss, use the same moves forward and backward, as the floss goes away from the tooth.In cases where spaces between teeth are wide should be used an interdental brush. The size of the brush should be tailored to each patient and should be used with soft movements of coming and going.
Contacts
-
Calçada de São Lourenço
N.º 3 1.º Andar D
9000-061 Funchal
Opening Hours
-
Monday – Friday
09h00 – 14h00
15h00 – 18h00
Saturdays, Sundays and Holidays
Closed
© Clínica de São Lourenço
Developed by Navega Bem Web Design


