- Home
- Treatments
- Temporomandibular Joint
Temporomandibular Joint
-
Temporomandibular Disorders
The temporomandibular joint corresponds to the jaw joint with the skull. The temporomandibular joint is one of the most complex of the human body and is responsible for moving the jaw forward, backward and sideways.
What are the temporomandibular disorders (TMD)?
Temporomandibular disorders relate to various problems affecting the temporomandibular joint and facial muscles. If you put your fingers in front of the ears and open your mouth you will feel the movement of the TMJ. It consists of a small ball, the condyle which articulates with another bone, the glenoid cavity through a small hard fibrous.
Several studies show that 20-30% of the population suffer from symptoms of TMD, apparently more women than men.
What are the causes of temporomandibular disorders?
 Trauma, either under the direct trauma or by prolonged clenching (bruxism);
Trauma, either under the direct trauma or by prolonged clenching (bruxism); Stress
Stress Malocclusion
Malocclusion Arthritis, TMJ
Arthritis, TMJ Tumors
TumorsMoreover, some general medical problems may affect the temporomandibular joint, such as rheumatoid arthritis or osteoarthritis.
Loss of Teeth
When multiple teeth are lost and not rehabilitated, the mandibular movement can alter the bite. This can overload the remaining teeth and over time can lead to both changes in the position of the teeth as the problems of the temporomandibular joint.
How is it diagnosed?
An important part of diagnosis is the history of the problem, when the symptoms began and whether they occur at certain times of day. The specialist will look for signs of wear and clenching and will palpate the muscles of mastication and neck and take x-rays to teeth and joints. You may need an MRI or a CT scan.
How is it treated?
The treatment of TMD depends on its cause. Most can be treated with a combination of the following:
 Soft diet
Soft diet Occlusal splint
Occlusal splint Analgesics
Analgesics Anti-inflammatory
Anti-inflammatory Muscle relaxants
Muscle relaxants Thermotherapy
Thermotherapy Laser
Laser Electrotherapy
Electrotherapy Orthodontic treatment
Orthodontic treatment Multidisciplinary oral rehabilitation.
Multidisciplinary oral rehabilitation.If conservative measures do not work and depending on your circumstances you may need surgical treatment.
Electrotherapy

-
Temporomandibular Joint Study and Rehabilitation Centre
What is the temporomandibular joint?
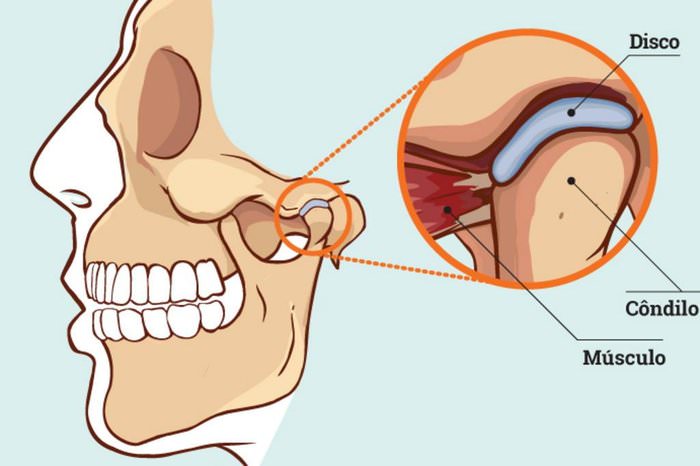
The temporomandibular joint frequently referred to as a TMJ, is a bilateral synovial joint, which connects the lower jaw (mandible) to the articular fossa of the temporal bone. The round upper end of the jaw, or movible portion of the joint is called the condyle; the socket is called the articular fossa. Between the condyle and the fossa is a disk made of cartilage that acts as a cushion to absorb stress and allows the condyle to move easily when the mouth opens and closes.
Function of the temporomandibular joint?
The TMJ allows the jaw to move smoothly up and down and side to side, enablying you to talk, make facial expressions, chew and yawn. The joint realizes between 1500 and 2000 movements daily.
What is a temporomandibular joint disorder?
A TMJ disorder refers to alterations of the jaw, TMJ and surrounding facial muscles.
Common symptoms include:- Clicking, popping or grating noises as you chew or move your mouth;
- Difficulty opening or closing the mouth;
- Radiating pain in the face, jaw or neck;
- Jaw muscle stifness;
- Difficulty chewing or a sudden uncomfortable bite, as is the upper and lower teeth are not fitting together;
- Jaws that get "stuck" or "lock" in the open or closed-mouth position.
Other symptoms may include: headache, earache, dizziness, upper shoulder pain, ringing in the ears.
Causes of a TMJ disorder:
In a healthy joint the end of the bones are covered with smooth cartilage, which allows them to glide easily when the jaw is moved. TMJ disorder can happen due to wear and tear of the cartilage; injuries; dislocations; damage to the surfaces of the teeth due to neglect or injury; bruxism (theet grinding) or overuse of facial muscles (due to stress, mouth breathing).
What is the treatment for temporomandibular joint disorders?
TMJ treatment may range from conservative dental and medical care to complex surgery; therefore, treatment should be accompanied by a multidisciplinary team of health care providers. An orthodontist may prescribe a stabilization splint and correct oclusal interferences when necessary. A physical therapist can develop a program for you that includes learning and practicing techniques for regaining normal jaw movement. The focus of the physical therapy for TMJ disorders is:
- Jaw excercises to strengthen muscles and improve flexibility and range of motion;
- Massage to relieve overall muscle tension;
- Training to improve posture and correct jaw alignement,
- Transcutaneous electrical nerve stimulation (TENS), which is the application of a mild electrical current to the skin over the jaw joint. It relaxes muscles, improves blood circulation, and relieves pain.
-
Bruxism
A parafunctional habit that occurs when the patient unconsciously grinds the teeth rhythmically during sleep or less harmfully, during the day.If the patient wakes up with sore jaw muscles and headaches he may be suffering from bruxism (clenching). Bruxism can cause pain and tooth mobility and loss of tooth structure by attrition. Can eventually destroy the gums and bone surrounding or lead to dysfunction of the temporomandibular joint.

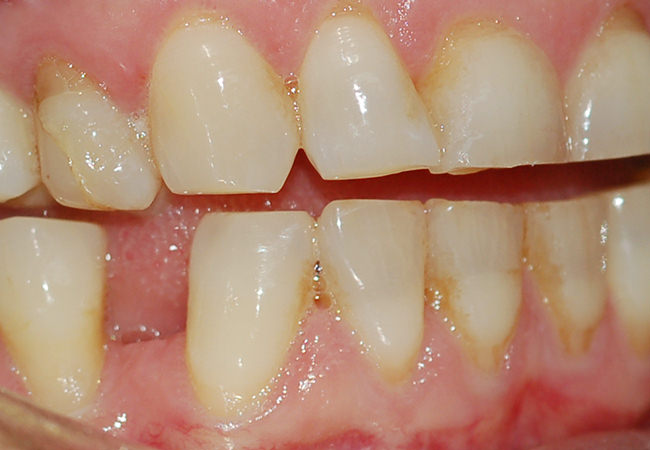
How to know if you have Bruxism?
For most people bruxism is an involuntary act and may not realize they do until someone heard the noise while sleeping or dentist / doctor alert them of the tooth wear. Other potential symptoms are pain in the face, head and neck.
How is bruxism treated?
The patient may be advised to sleep with an occlusal splint. This device is made starting from a model of the patient's teeth and covers the upper teeth, thus preventing them to wear. This product only reduces tooth wear but does not cure bruxism so it's very important to minimize stress (responsible for bruxism). It is also very important to improve the occlusion (bite) through orthodontics, crowns or elimination of premature contacts.
Contacts
-
Calçada de São Lourenço
N.º 3 1.º Andar D
9000-061 Funchal
Opening Hours
-
Monday – Friday
09h00 – 14h00
15h00 – 18h00
Saturdays, Sundays and Holidays
Closed
© Clínica de São Lourenço
Developed by Navega Bem Web Design


